A foot above the rest: tread more comfortably thanks to Feet First Podiatry
It would hardly be an exaggeration to claim the majority of us take our feet for granted, not putting them first in our health and wellbeing regimen. Charlotte Russell of Feet First Podiatry says that treating feet is not a luxury, but rather a necessity. A podiatrist for more than 30 years, Charlotte knows what […]
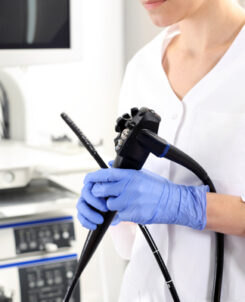
An indigestible condition: Surgeon Ross Roberts from The Endoscopy Clinic on gastric reflux
Eating and drinking are some of the most basic human needs and yet, for many people who suffer from chronic and repeated gastric reflux, the freedom to eat and drink what they choose may not be a given. Metropol talks to endoscopy specialist, Surgeon Ross Roberts from The Endoscopy Clinic about gastric reflux and what […]
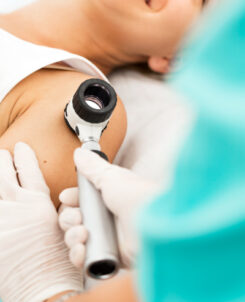
Early detection does matter: Molecheck and why you should get your skin checked sooner rather than later
Just like blood pressure, mammograms or a dental checkup, it’s important to monitor your skin’s health. As we say goodbye to summer, it’s time to tick off your skin check as well. Early detection matters. We’ve enjoyed the sunshine, now we should check what damage it may have caused. Even though skin cancer is usually […]
Aneurysm risk & assessment: Christchurch Vascular Group want to help you look after yourself and your loved ones
It’s a fancy word, but an aneurysm is simply a dilated blood vessel. As the blood vessel dilates, there is an increased risk of complications such as thrombosis or rupture. If the abdomen’s main blood vessel – the aorta – becomes dilated or greater than 30mm, it is called an Abdominal Aortic Aneurysm or AAA, […]
A fulfilled life : Wigram Health on being proactive with your health
Whether you are a busy executive, retiree or working parent, your health is important. Each of these important life stages are a crucial time to take care of yourself, because optimal health is vital to leading an active and meaningful life. At Wigram Health, patient health is the dedicated team’s top priority. The team understands […]
Massage magic: a relaxing visit to Beauty Progress
Would you be interested in better health, more relaxation, better circulation, greater flexibility, higher levels of peace of mind, an improved sense of well-being, stress relief and a feeling of being totally revitalised? A visit to Beauty Progress Thai Massage Spa for a traditional Thai Massage is designed to re-energise your body, mind and soul. […]
Exceptional eye care: why Corneal Lens Corporation is so excited about their newly stocked Evolve range of eye drops (and why you should be too!)
Christchurch’s Corneal Lens Corporation is thrilled to welcome the Evolve range of eye drops for dry eyes. Created and manufactured in London, Evolve Eye Drops quickly became a top seller in the UK, prompting Corneal Lens Corporation to bring the premium products to New Zealand. Whitney Parsons, Marketing and Accounts Manager for Corneal Lens Corporation, […]